Anna, 32
Urine leakage during physical activity, sneezing, laughter — appeared after a second delivery.
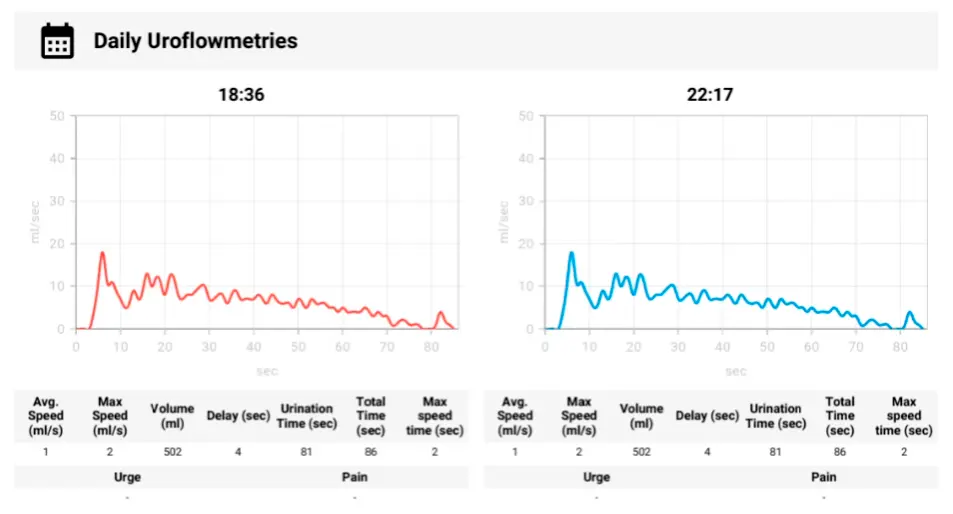
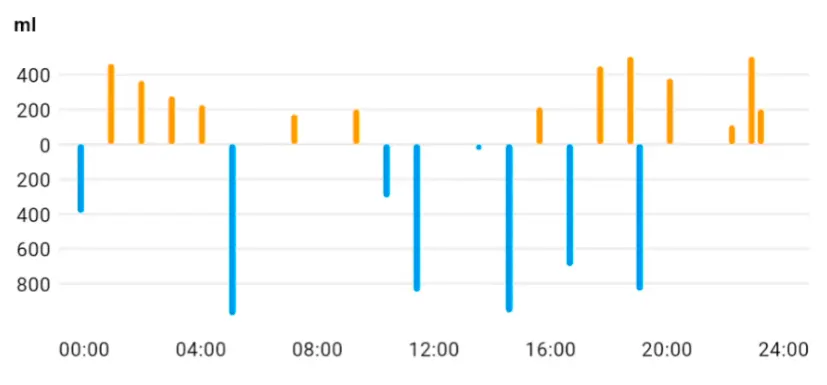
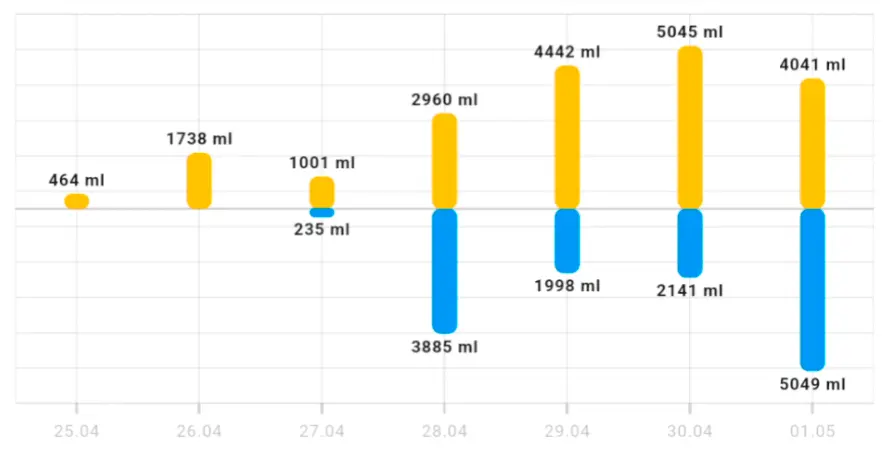
Recorded frequency and circumstances of episodes — exertional situations, morning hours. Three-day data showed 4–6 episodes per day.
Pelvic floor exercise programme (Kegel) prescribed. Diary used to assess progress at 4 weeks.